The proliferation of online information in the digital age is a boon and a curse — a curse, because of how prevalent misinformation has become. One of the most widespread brain health misbeliefs rife across social media is: “because the brain is primarily made up of fat, it stands to reason that it would thrive on a high-fat diet.”
There is a kernel of truth here: our brains do indeed require fat. But there are many different types of fat, and not all variations grant the same health benefits. Let’s investigate.

How much of the brain is made up of fat?
Sat inside our skulls, the human brain is a marvel of complexity and functionality that’s made up of around 60% lipids (fats) in terms of dry weight.
These fats serve a number of indispensable roles within the brain, including formation of the cell membranes and production of myelin: the fatty, insulating sheath encircling nerve fibers.
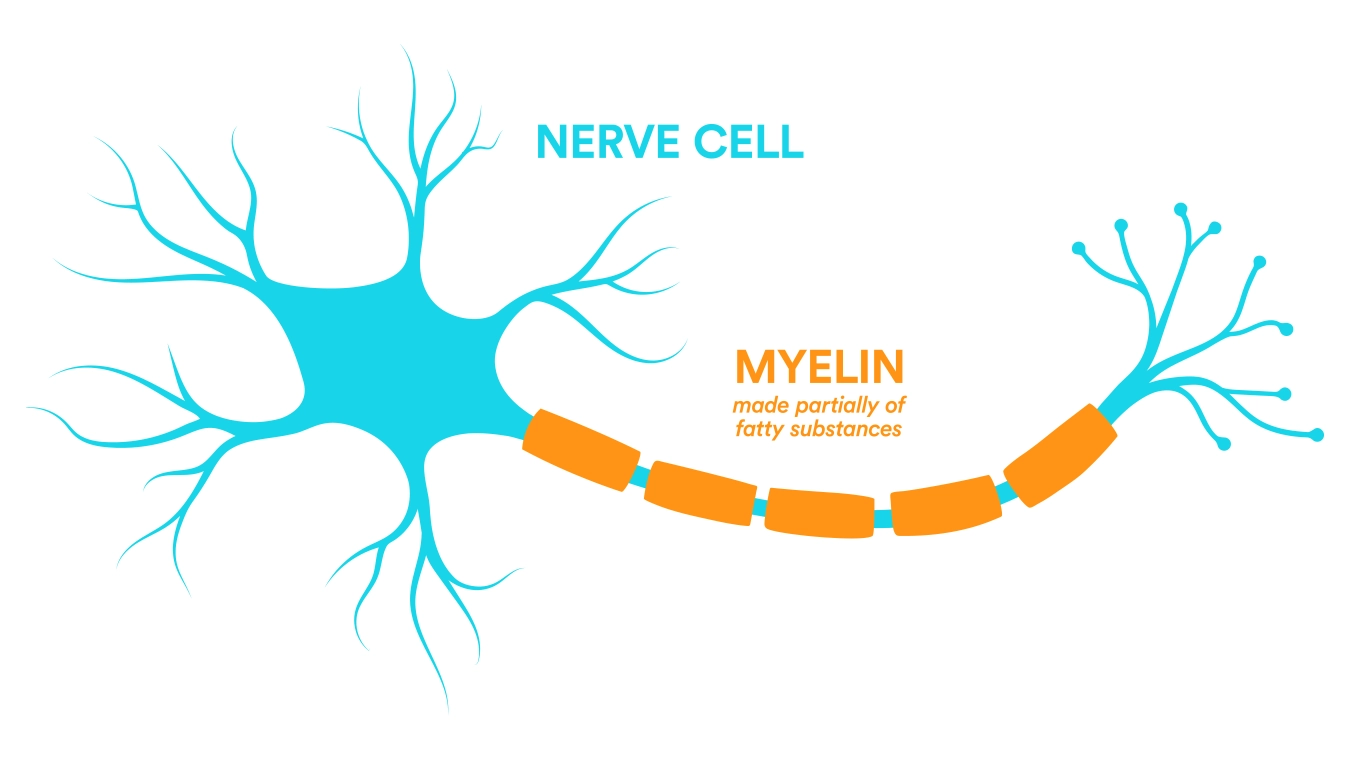
This insulation permits swift and efficient transmission of electrical impulses along nerve cells, facilitating everything from thought processes to coordination and sensory perception.
One particular lipid, docosahexaenoic acid (DHA), holds special importance in this context. DHA is a type of omega-3 fatty acid and a primary structural component of the human brain.
About 30% of the structural lipid in grey matter is DHA — it’s integral to the health of neurons, the core communicators in our brains.
DHA’s presence is crucial to learning capabilities, memory retention, and overall brain health.
What’s the difference between brain fat and ‘body’ fat?
When we talk about our brain as being made of fat, it’s important to note that this doesn’t mean the brain contains ‘fat stores’ similar to other parts of our body.
Unlike adipose tissue, which primarily serves as energy storage, the lipids in the brain are integral components of its cellular structure — vital for its complex communication networks.
The brain doesn’t have pockets of ‘unused’ fat, as is the case for other parts of the body. Each lipid molecule has a role in the structure or function of the organ.
Also, it should be noted that dietary fats can’t cross the blood-brain barrier: an extensive membrane that regulates the passage of substances from the blood into the brain.
Fats, proteins, and other large molecules can’t freely cross this barrier, but glucose, amino acids, and certain other small molecules can, allowing them to nourish brain cells.
Interestingly, the brain is capable of synthesizing all the lipids it needs, except for DHA. This fact highlights the importance of dietary DHA for brain health.
Since the brain cannot produce DHA, and DHA cannot easily cross the blood-brain barrier, the body has to convert dietary DHA into a form that can be transported across the barrier to nourish the brain.
So, to view our brain as a ‘blob of fat’ that stands to gain from a high-fat diet is a gross oversimplification, and a potentially harmful idea to spread on social media.
Such a reductionist perspective fails to account for the complexity of our brain’s structure, the role of different fats in brain health, and the way nutrients interact with our unique neurobiology.
A more nuanced understanding can guide healthier dietary choices and support our brain’s critical functions.

Why saturated fats can harm the brain
Saturated fats, which are ubiquitous in foods like red meat, full-fat dairy, and plant-based sources such as coconut oil and palm oil, have been intensely scrutinized for their potential adverse effects on human health.
They’ve been linked to an increased risk of cardiovascular disease, a claim backed by decades of research. The ‘Seven Countries Study’ by Ancel Keys, which started in the 1950s and followed subjects for over 25 years, was among the earliest to associate saturated fats with heart disease, providing the bedrock for subsequent research in this field.
However, more recent research has started to delve into the potentially detrimental effects of saturated fats on brain health. A study published in ‘Annals of Neurology’ in 2012 found that high intake of saturated fats may accelerate the progression of Alzheimer’s disease.
In this study, people who consumed the most saturated fat had two times the risk of developing Alzheimer’s disease compared to those who ate the least.
Why does high consumption of saturated fats contribute to cognitive decline? Because they increase the levels of low-density lipoprotein (LDL) cholesterol in the blood. LDL, often referred to as ‘bad cholesterol’, has been implicated in both cardiovascular disease and stroke. Elevated LDL levels can increase the risk of small vessel disease, a condition characterized by damage to the small blood vessels in the brain. This can eventually lead to cognitive deterioration and an increased risk of stroke and dementia.

A diet high in saturated fats can also exacerbate inflammation and oxidative stress — an imbalance between the production of free radicals and the body’s ability to counteract their harmful effects. Both inflammation and oxidative stress are predominant factors of the onset and progression of neurodegenerative diseases. This association provides another worrying link between saturated fats and brain health.
Numerous epidemiological studies also hint at the connection between a diet rich in saturated fats and Alzheimer’s disease. For instance, a study published in ‘JAMA Neurology’ in 2003 found that a high intake of saturated fats doubled the risk of Alzheimer’s disease in a group of 815 individuals aged 65 and older, over a four-year period.
Therefore, it becomes clear that the excessive consumption of saturated fats could be detrimental not just to our cardiovascular health but to our brains as well.
Our understanding of the link between diet and brain health is continually evolving, but the evidence so far emphasizes the importance of managing saturated fat intake to protect our cognitive wellbeing.

BRAIN-HEALTHY RECIPE
Strawberry Rose Chia Puding
Chia seeds are an incredible source of omega-3 fatty acids, which have been linked to reduced risk of cognitive decline and dementia. One of our favorite ways to consume them is in our incredible and easy-to-make Strawberry Rosa Chia Pudding.
Why polyunsaturated fats can benefit brain health
In contrast to saturated fats, polyunsaturated fats — especially omega-3 fatty acids — have emerged as vital nutrients for brain health.
Docosahexaenoic acid (DHA), the omega-3 fatty acid I mentioned earlier, is an integral structural component of the brain and retina. It plays a pivotal role in maintaining brain function and cognition.
Contemporary research, including a comprehensive review by myself and my and colleagues, highlights the neuroprotective properties of omega-3s, and suggests they may enhance cognitive function.
In our review titled ‘The Omega-3 Fatty Acids EPA and DHA in Brain Aging’, published in the Journal of Nutrition, Health & Aging, Sherzai et al. highlight the importance of these fatty acids for the aging brain. We present compelling evidence from various epidemiological studies and clinical trials linking dietary omega-3 intake — DHA specifically — with a lower risk of cognitive decline and dementia.
One study, published in Annals of Neurology in 2012, found that a higher intake of omega-3 fatty acids was associated with a larger total cerebral brain volume, suggesting their protective effect against brain aging. And another study, published in The Journal of Neurochemistry in 2001, suggested that DHA plays a critical role in neuronal function and survival, and that dietary DHA could potentially delay the onset of Alzheimer’s disease.
Omega-3 fatty acids also contribute to the fluidity of cell membranes, promote neuronal communication, and counteract inflammation, thus proving how crucial their role is in maintaining a healthy brain.

Which diets include healthy fats?
These beneficial brain-healthy fats can be obtained from a diet rich in fatty fish like salmon and mackerel, walnuts, flaxseeds, and chia seeds.
It’s worth noting that while some studies, such as the PREDIMED trial, suggest that Mediterranean diets (known to be high in fish and thus omega-3 fatty acids) are associated with better cognitive function and a lower risk of dementia, the underlying protective mechanism may not be solely due to fish consumption.
Several other components of the Mediterranean diet, such as high consumption of fruits, vegetables, whole grains, and legumes, and the overall balance of polyunsaturated to saturated fats, are also likely to contribute to these beneficial effects.
As such, while fish is indeed a source of omega-3 fatty acids, the protective effect of a diet against cognitive decline and dementia may hinge more significantly on the overall dietary pattern, particularly the ratio of polyunsaturated to saturated fats.
This insight underlines the importance of a predominantly plant-based diet that’s rich in nutrients for sustaining brain health and thwarting neurodegenerative diseases.
- A plant-based diet abundant in fruits, vegetables, whole grains, legumes, and nuts can provide a rich assortment of essential nutrients, while keeping saturated fat intake to a minimum
- Omega-3 fatty acids — crucial for brain health — can be incorporated through fish in those who include it in their diet, but can also be derived from various plant sources such as flaxseeds, chia seeds, hemp seeds, and walnuts
- For those with dietary restrictions or preferences, or in cases where dietary intake may not be sufficient, supplementation with omega-3 fatty acids can be considered, under the guidance of healthcare professionals

The dangers of diet and health misinformation
The “your brain is made of fat, therefore, it needs lots of fat” assertion is a gross oversimplification that could potentially mislead the public in dangerous ways.
While it is correct that the brain requires certain types of fat, it is misguided and potentially harmful to imply that all fats are uniformly beneficial.
A growing body of evidence-based consensus indicates that a diet rich in saturated fats can be detrimental to both brain health and general wellbeing, and that a diet incorporating adequate omega-3 fatty acids can bolster brain function and overall health.
As a society, it is our collective responsibility to debunk nutritional myths surrounding brain health and champion the importance of a well-rounded, balanced diet rich with essential nutrients.
Medical professionals, researchers, educators, and policy-makers must take a front seat in dispelling these misunderstandings, and should share clear, science-backed dietary guidelines. Our brains’ health, and by extension our overall health, hangs in the balance.
Circulation of accurate information about dietary fats transcends mere myth-busting. It lies at the heart of preventing and managing a host of prevalent diseases. Armed with science-backed knowledge, we can make informed dietary choices and commit to nurturing our health and wellbeing.
References
Keys, A., Menotti, A., Karvonen, M. J., Aravanis, C., Blackburn, H., Buzina, R., … & Puddu, V. (1986). The diet and 15-year death rate in the seven countries study. American Journal of Epidemiology, 124(6), 903–915.
Morris, M. C., Evans, D. A., Bienias, J. L., Tangney, C. C., Bennett, D. A., Aggarwal, N., Schneider, J., & Wilson, R. S. (2003). Dietary fats and the risk of incident Alzheimer disease. Archives of Neurology, 60(2), 194-200.
Okereke, O. I., Rosner, B. A., Kim, D. H., Kang, J. H., Cook, N. R., Manson, J. E., Buring, J. E., Willett, W. C., & Grodstein, F. (2012). Dietary fat types and 4-year cognitive change in community-dwelling older women. Annals of Neurology, 72(1), 124-134.
Bowman, G. L., Silbert, L. C., Howieson, D., Dodge, H. H., Traber, M. G., Frei, B., Kaye, J. A., Shannon, J., & Quinn, J. F. (2012). Nutrient biomarker patterns, cognitive function, and MRI measures of brain aging. Neurology, 78(4), 241-249.
Sherzai, A., Sherzai, D., Li, J., & Singh, I. (2018). The Omega-3 Fatty Acids EPA and DHA in Brain Aging. Journal of Nutrition, Health & Aging, 22(3), 474-485.
Salem, N. Jr, Litman, B., Kim, H. Y., & Gawrisch, K. (2001). Mechanisms of action of docosahexaenoic acid in the nervous system. Lipids, 36(9), 945-959.
Martínez-Lapiscina, E. H., Clavero, P., Toledo, E., Estruch, R., Salas-Salvadó, J., San Julián, B., Sanchez-Tainta, A., Ros, E., Valls-Pedret, C., & Martinez-Gonzalez, M. Á. (2013). Mediterranean diet improves cognition: the PREDIMED-NAVARRA randomised trial. Journal of Neurology, Neurosurgery & Psychiatry, 84(12), 1318-1325.

About The Author
Dean Sherzai, MD, PhD
Dr. Dean Sherzai is co-director of the Alzheimer’s Prevention Program at Loma Linda University. Dean trained in Neurology at Georgetown University School of Medicine, and completed fellowships in neurodegenerative diseases and dementia at the National Institutes of Health and UC San Diego. He also holds a PhD in Healthcare Leadership with a focus on community health from Andrews University.
Get more brain science direct to your email inbox
Sign up for the Brain Docs newsletter for weekly recipes, brain teasers, neuroscience facts, podcast updates, and more — for free!




